If you are unable to find an available LifeLabs appointment slot to get your blood drawn in the next two business days, please contact our customer care line for further booking support, using one of the following numbers: 1-877-849-3637 (Ontario), 604-431-7206 (British Columbia) or 1-888-333-0222 (Saskatchewan).
Why choose Panorama™?

- Panorama™ can be ordered as early as 9 weeks**, giving you time to plan and prepare for your baby
- Panorama™ carries no risk of miscarriage, and reduces unnecessary invasive procedures like CVS and amniocentesis
- Panorama™ can tell you the sex of your baby (optional), and has zero sex determination errors in validation studies
- Panorama™ screens for Down Syndrome with an accuracy of greater than 99%
- Panorama™ can screen for common microdeletions that impact all pregnancies equally regardless of maternal age
- Panorama™ is the only prenatal screen that detects and differentiates between DNA from mother and baby, resulting in greater accuracy
- Panorama™ can tell you if your twins are identical or fraternal, and report the sex of each fetus
- Panorama™ results are available to your ordering health care provider within 7-10 days* of being received in the laboratory.
- Panorama™ results are available for patients through LifeLabs’ online portal 5 calendar days after the report is released to the ordering health care provider.
*Closures during holidays may affect reporting times
**Must be at least 9 weeks gestation. Samples collected before 9 weeks will require a repeat collection.
We are here for you every step of the way.
LifeLabs’ Genetic Counsellors are available to answer questions before or after you make a decision to proceed with a Panorama screening test.
Connect with the Genetics team
Email: Ask.Genetics@Lifelabs.com
Phone: 1-84-GENE HELP (1-844-363-4357)

Watch our videos, starring one of our very own Genetic Counsellors, Ruth!
Book an appointment for your
Panorama™ test today!
To find a location:
Ontario, British Columbia and Saskatchewan locations
Quebec locations
All other provinces
please contact
1-84-GENE HELP
(1-844-363-4357).
What does Panorama™ tell me?
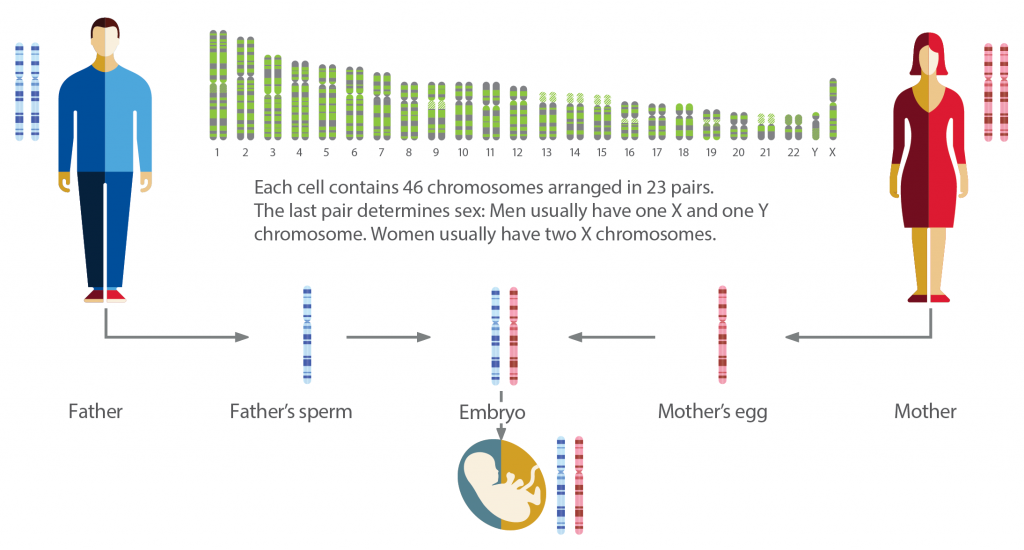
Chromosomes are the structures inside the cells of the body.
They contain our DNA, or genetic code, which tells the body how to grow and develop.
A mother and father each contribute one chromosome through the egg and sperm. Typically, the egg and sperm each contain 23 chromosomes. When they combine at fertilization, an embryo is formed, which normally has the right number of chromosomes: 23 + 23 = 46.
When there’s a difference in the usual number of chromosomes, it is called an aneuploidy
- An extra copy of any one chromosome — 3 copies instead of 2 — is called a trisomy (tri-meaning “three”)
- A missing copy of any one chromosome — 1 copy instead of 2 — is called a monosomy (mono-meaning “one”)
Types of aneuploidies
There are many different types of aneuploidies that require clinical care by a physician or other healthcare
professional. Panorama can provide a risk score for the following:
Trisomy 21:
Down Syndrome
- Approximately 1 in 700 babies is born with Down syndrome1.
- The chance of miscarriage is higher: up to 30%
Children born with Down syndrome typically have some intellectual differences and characteristic physical features, and may have birth defects involving the heart and other organs. They will need extra medical care depending on the child’s specific health problems.
Most people with Down syndrome live into their 60s.
Trisomy 18:
Edwards Syndrome
- Approximately 1 in 3,000 babies is born with Edwards syndrome1
- The chance of miscarriage is higher: 60%–70%
Babies with Edwards syndrome often have severe intellectual differences and life-threatening birth defects; fewer than 10% live beyond 1 year old.
Trisomy 13:
Patau Syndrome
- Approximately 1 in 5,000 babies is born with Patau syndrome1
- The chance of miscarriage is higher: 60%–70%
Babies with Patau syndrome often have severe intellectual disabilities and life-threatening birth defects involving the heart and brain; only 5%–10% live beyond 1 year old.
Monosomy X:
Turner Syndrome
- Approximately 1 in 2,500 girls is born with Turner syndrome1
- A large proportion of pregnancies will result in a miscarriage in the first or second trimester
Girls with Turner syndrome:
– may have mild or more severe health problems, including heart defects, kidney problems, hearing problems, and minor learning differences
– usually experience premature ovarian failure; they do not go through puberty or produce eggs on their own
Sex chromosome:
trisomies
- Approximate number of babies born with sex chromosome trisomies (when there is an extra copy of one of the sex chromosomes):
- Klinefelter syndrome (XXY): 1 in 1,0001
- Triple X syndrome (XXX): 1 in 8001
- Jacob’s syndrome (XYY): 1 in 650 boys1
Most children with sex chromosome trisomies have intelligence in the normal range but have a higher chance of learning differences 2, for which early intervention can be helpful 3.
1. Nussbaum et al. 2007 Thompson and Thompson Genetics in Medicine (7th Ed.) Oxford Saunders, Philadelphia, PA
1. Arthur Robinson & Mary G. Linden, 1993, Clinical Genetics Handbook (2nd Ed.). Cambridge, Mass., Blackwell Scientific Publications
2. Tartaglia et al. J Dev Behav Pediatr. 2012 May;33(4):309-18. 3. Linden, Bender. Am J Med Genet 2002 Jun 1;110(1):11-8.
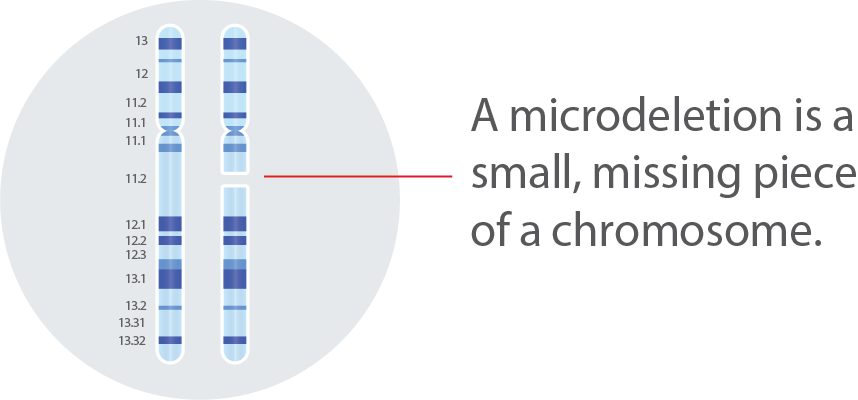
Five of the more well-known microdeletions
| Syndrome | Incidence |
|---|---|
| 22q11.2 deletion/ DiGeorge |
1 in 1,524 1 |
| Prader-Willi | 1 in 10,000 2 |
| Angelman | 1 in 12,000 3 |
| Cri-du-chat | 1 in 20,000 4 |
| 1p36 deletion | 1 in 5,000 5 |
- Certain types of microdeletions can cause health problems for the baby that may need immediate care upon birth.
- Early screening can guide the management of the pregnancy or allow decisions for the delivery and special needs of your child.
- Babies with 22q deletion syndrome, for example, have a harder time maintaining calcium in their bodies — so prenatal testing ensures doctors know they need to monitor your child’s levels from birth and supplement as necessary.
- Note: Microdeletions are present from conception and not a result of anything you or your partner did or didn’t do.
1. https://doi.org/10.1016/j.ajog.2022.01.002.
2. www.ncbi.nlm.nih.gov/books/NBK1330.
3. www.ncbi.nlm.nih.gov/books/NBK1144.
4. Niebuhr, E. The cri du chat syndrome: epidemiology, cytogenetics, and clinical features. Hum. Genet. 44: 227-275, 1978.
5. www.ncbi.nlm.nih.gov/books/NBK1191.
Panorama's Full Prenatal Panel includes the following microdeletions:
22q11.2 Deletion syndrome/DiGeorge syndrome

1p36 deletion syndrome

Angelman syndrome

Cri-du-chat syndrome, also known as 5p minus

Prader-Willi syndrome


22q11.2 Deletion syndrome/DiGeorge syndrome

1p36 deletion syndrome

Angelman syndrome

Cri-du-chat syndrome, also known as 5p minus

Prader-Willi syndrome

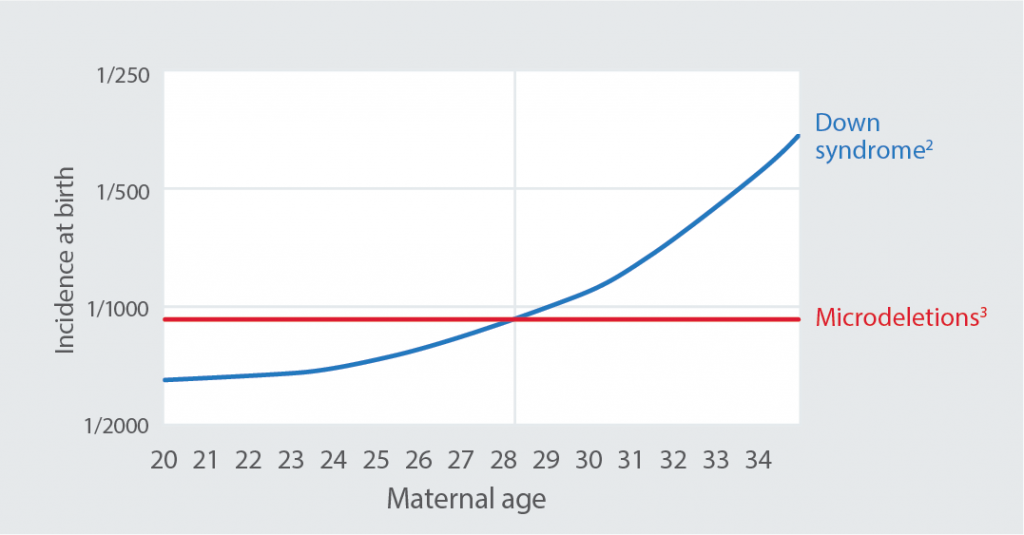
Maternal age and risk for trisomies 21, 18, and 13
- The rate of non-disjunction in eggs increases with maternal age; thus the number of pregnancies with chromosome aneuploidies increases with maternal age.
- The combined chance of all chromosome aneuploidies decreases with gestational age because some pregnancies will be miscarried as a result of the chromosome difference.Maternal age and risk for trisomies 21, 18, and 13
Maternal age and risk for monosomy and triploidy
- There is no increased chance of monosomy X or triploidy as maternal age increases.
Maternal age and risk for microdeletions
- Microdeletions occur randomly (which means they don’t run in families) and equally affect any baby regardless of race or maternal age.
Microdeletions are not affected by maternal age, and are more common than Down syndrome in younger women.
1. Modified from Hook EB. Chromosomal abnormalities: prevalence, risks and recurrence. In Prenatal Diagnosis and Screening. Edinburgh: Churchill Livingstone 1992; 351-392. & Hook EB, et al. Rates of chromosome abnormalities at different maternal ages. Obstet Gynecol:1981, 58(3);282-5.
2. Snijders RJ, et al. Ultrasound Obstet Gynecol. 1999 Mar; 13(3): 167–70.
3. Combined prevalence using higher end of published ranges from Gross et al. Prenatal Diagnosis. 2011; 39:259-266; and from www.genetests.org. Total prevalence may range from 1/1071–1/2206.
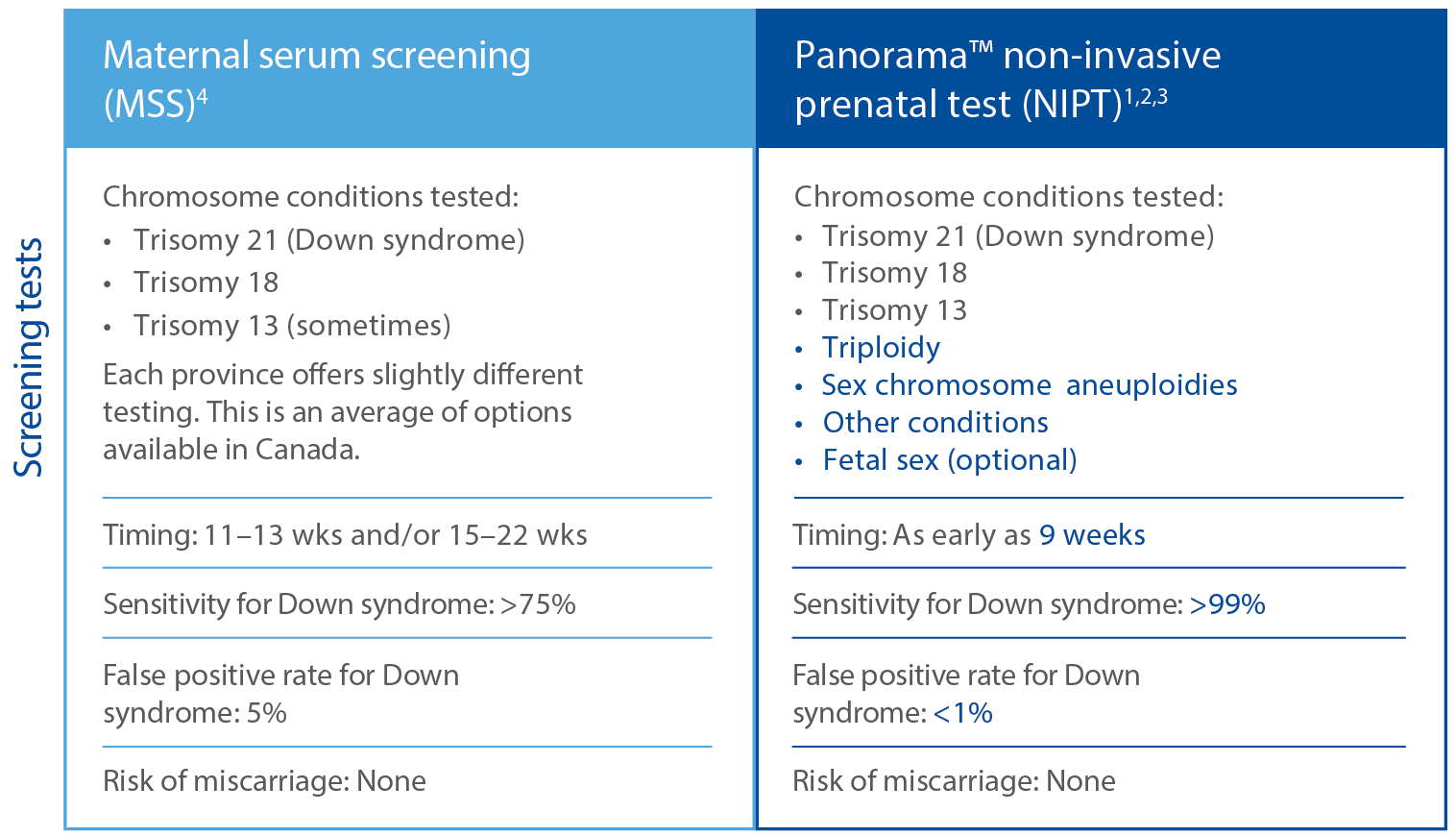
So why should I order Panorama™ when I get maternal serum screening done
through the provincial healthcare system?
Chances are, your baby will be born perfectly healthy! Most prenatal screening tests are an optional part of
your pregnancy care plan – but well worth your consideration.

A detailed ultrasound is still recommended for all patients, regardless of screening option.
Ultrasound provides important information on the growth and development of the fetus.
1. Nicolaides, et al. Prenat Diagn. 2013 Jun; 33(6):575-9. doi: 10.1002/pd.4103. 2. Pergament et al. Obstet Gynecol. 2014 Aug; 124(2):210-218. 3. Ryan, et al. FetalDiagn Ther. 2016; 40(3):219-23. doi: 10.1159/000442931. . 4. Norton et al. N Engl J Med. 2015; 372:1589-1597. 5. ACOG/SMFM, practice bulletin #162, May 2016.
Maternal Serum Screening (MSS)

Panorama NIPT

1. Norton et al. NEJM. 2015 Apr 23; 372(17):1589-97. 2. Dar et al. Am J Obstet Gynecol. 2014 Nov; 211(5):527.
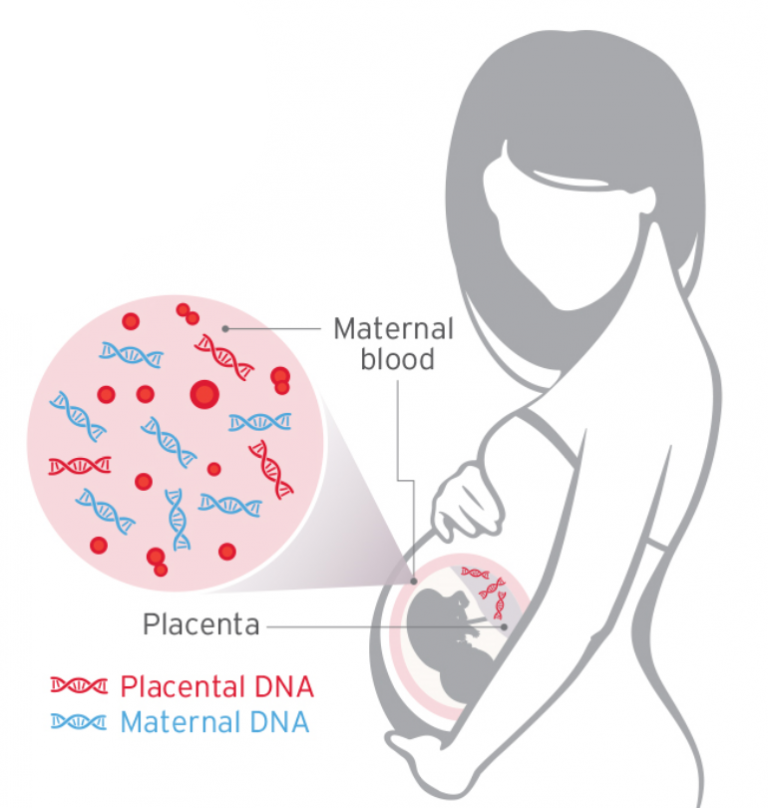
NIPT, non-invasive prenatal testing (also called cell-free fetal DNA testing) uses a blood sample from the mother to analyze DNA from the placenta for certain chromosome conditions, like Down syndrome, that could affect the baby’s health.
How does NIPT work?
- There are always pieces of genetic information (cell-free DNA) floating in our bloodstreams.
- When a woman is pregnant, pieces of genetic information from the placenta (cell-free fetal DNA) are released into her bloodstream and mix with her own genetic information.
- NIPT tests the mixture of DNA to determine if there is a high or low risk that the baby has certain chromosome anomalies.
- Fetal fraction, or the proportion of DNA in the blood sample that comes from the placenta, can affect the accuracy of an NIPT test.
Panorama™ offers patients a personalized risk score. It is a screening test, not a diagnostic test.
Your report may state the following:



• If fetal sex option was selected on the requisition form, it will be included in the results
• If the full panel with microdeletions was added, the risk for individual anomalies will be included in the results
Due to Panorama’s unique SNP-based technology, it is the only NIPT test that:
- Differentiates between mom and baby
- Can detect triploidy and molar pregnancies that may result in complications
- Can detect a demised twin, a common cause of false positive results
- Has zero errors in determining fetal sex
- Reports whether twins are identical or fraternal
- For identical twins, can detect sex chromosome trisomies, monosomy X, and 22q11.2 deletion syndrome for each twin

Panorama™ is appropriate for singleton or twin pregnancies, as well as singleton pregnancies conceived using egg donors or surrogates. This test is not informative in pregnancies with 3 or more fetuses, nor for women who have had a bone marrow transplant.
| Basic Prenatal Panel | $550 | Trisomy 21, 18, 13, monosomy X, sex chromosome trisomies, triploidy, complete molar pregnancy and fetal sex optional |
| Extended Prenatal Panel | Was |
Basic Prenatal Panel, plus 22q.11.2 [DiGeorge Syndrome]. |
| Full Prenatal Panel | $795 | Basic Prenatal Panel, plus 5 microdeletions (22q.11.2 [DiGeorge syndrome], 1p36 deletion syndrome, Angelman syndrome, Cri-du-chat syndrome, Prader-Willi syndrome) |
FORMS AND DOCUMENTS
Requisition & Patient Consent Forms
|
LifeLabs Private-Pay Requisition for Panorama |
Payment Form
| Private-Pay Payment Form for Panorama English | French |
Requisition Change Form
| Change Authorization Form |
Sample Reports
LEARNING
|
Patient Brochure Panorama™ NIPT Patient Pamphlet in English, French, Hindi, Chinese and Arabic Physician Detail Aid Panorama™ Physician Detail Aid in English, French 22q11.2 Deletion Syndrome SMART Detail Aid SMART Data Physician Detail Aid in English News Temporary Pandemic MOH Coverage of NIPT for Twin Pregnancies Now Permanent as of December 17, 2021 Prenatal Screening Ontario: NIPT Funding Criteria Get Peace of Mind About the Health of Your Baby Early in Pregnancy Podcast Dawn Siciliano talks to She Found Motherhood in episode Prenatal Screening in Pregnancy: What are my options??? |
Videos
“All I Want Is to Be Prepared”
How do I order this test?
OR
Talk to your doctor:
Download this information package to learn all you need to know about Panorama™. It can be used to help guide the discussion with your doctor, and includes the Panorama™ patient brochure and requisition form.